The Role Of Seed Funding For Alleviating Blindness In Poor Communities
During my fifteen years as a technology investor and advocate of the prospect of artificial intelligence to improve human life I have been proud to back some amazing ventures. And recently the same ‘portfolio’ approach that I have typically applied to my investments has been proving equally effective for allocating resources to my philanthropic objectives. This is not a great new discovery. The Bill and Melinda Gates Foundation has been doing it for well over a decade. But in the field of ophthalmology and corneal blindness, it remains somewhat novel.
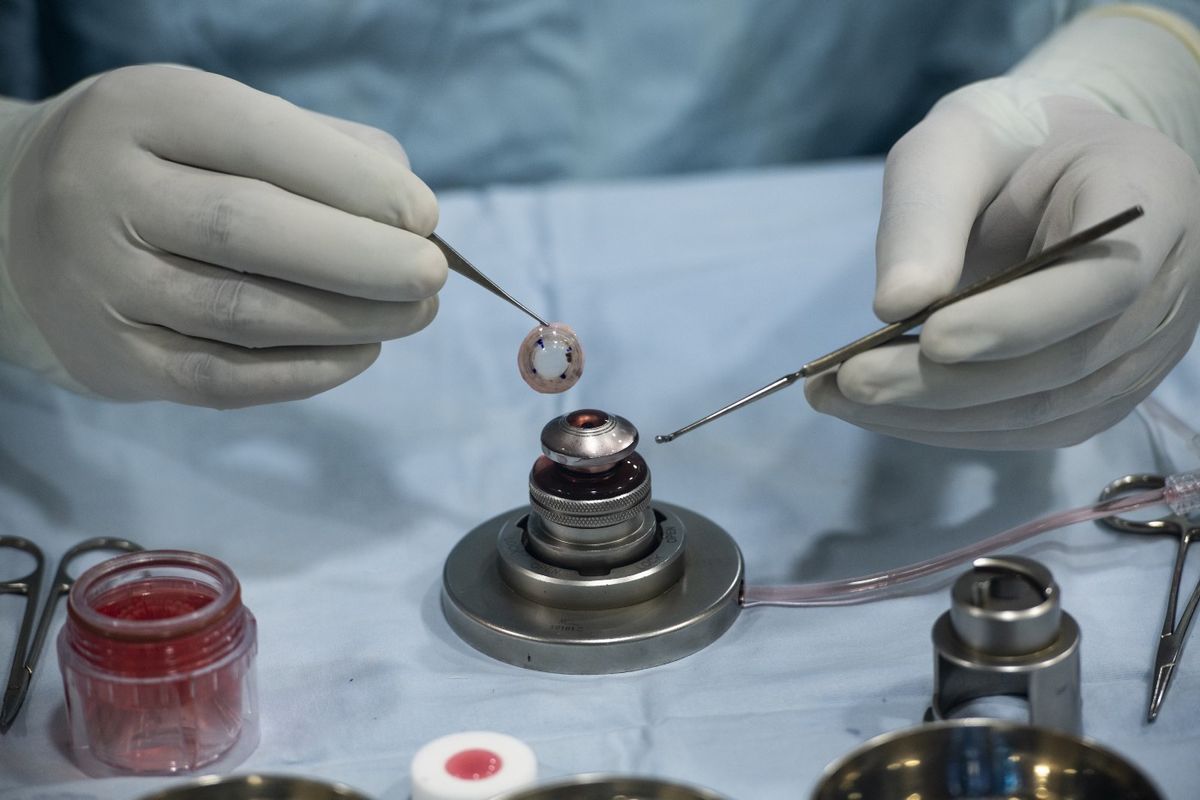
Between 2015 and 2019 I funded extensive measures for the prevention, treatment and cure of corneal blindness and severe visual impairment. In 2019 5,736 people had their blindness cured at the Tej Kohli Cornea Institute. The YouTube channel of the Tej Kohli Foundation is filled with the stories of individuals and families who have been cured. But the harsh reality has always been that because 90% of those suffering needlessly with corneal blindness live in the poorest countries in the world, most do not have access to affordable treatment.
This is why I have long advocated the development of an accessible, affordable and scalable solution to corneal blindness that could be applied in these poorer communities. Corneal transplantation is too complex and expensive to reach all of those in need, so brand new innovations are needed. In recent years the Tej Kohli Foundation Applied Research program has been moving nearer to a scalable universal solution to end corneal blindness that could be applicable in these poor and underserved communities; and in 2019 I donated $2m to Mass Eye and Ear in Boston, a teaching hospital of Harvard Medical School, to support further innovations. I have also sought incubate brand new projects that have a clear pathway to ending blindness regardless of whether they were commercial or not-for-profit.
The Tej Kohli Foundation publicises some of these efforts because invariably the projects are multidisciplinary and involve input from many institutions and experts from around the world. As was noted in a recent Financial Times Special Report on regenerative medicine to cure blindness, my Tej Kohli Foundation Applied Research program alone has collaborators in Montreal (Canada), Odessa (Ukraine) and Hyderabad (India) as well as London’s Moorfields Eye Hospital and the UCL Institute of Ophthalmology. Bringing together all of these different parties to collaborate does not happen organically. It comes from the regular sharing of stories and successes.
And it’s because of this sharing process that new projects are created which promise to offer new solutions for the alleviation and cure of corneal blindness. The difficult question then becomes, which projects should be backed, and which should not? This is when seed funding becomes useful. Seed funding provides enough resources for these projects to prove their viability. But to receive any further funding, projects must prove that they can make a real difference to ending blindness in poor communities.

This is particularly important for me. Throughout history, brand new innovations tend to first manifest as expensive indulgences for the wealthy. We see this regularly with the advent of new technologies. We’re seeing it now in healthcare with treatments like CAR T-cell therapy proving too expensive to scale to everyone despite its incredible efficacy in curing cancer. Invariably these innovations eventually become ‘democratised’ and accessible to all, but the question is, how quickly? When looking at projects to end corneal blindness in poor communities, I have to balance the immediate scientific and clinical merits of a project with the likelihood that it can be ‘democratised’ to serve poor communities before my 2035 target. Seed funding gives these projects enough latitude to show whether they can help meet this target.
Recently the Tej Kohli Cornea Program at Mass Eye and Ear, a teaching hospital of Harvard Medical School in Boston, has allocated seed funding to two new research initiatives as it pursues new innovations to cure corneal blindness. The research projects will be led by investigators from the Harvard Medical School Department of Ophthalmology. Both seed projects have the potential promise to help alleviate blindness in poor communities.
The first project to receive seed funding from the Tej Kohli Cornea Program in Boston will focus on preventing corneal endothelial cell loss. Corneal endothelial cells (‘CEC’) are situated in the back portion of the cornea and keep the cornea clear through the constant pumping of ions. Currently there are no effective medical therapies to prevent or restore CEC loss. The research project will utilize new technology for the regeneration of CECs by utilizing small molecules to augment mitochondrial viability to promote native stem cell growth and prevent cell death.
Loss of CECs occurs from ageing, cataract surgery, infection, attrition and dystrophy. This CEC loss is usually permanent and leads to corneal swelling and blindness. Importantly, CEC loss is one of the leading reasons that a patient might need a corneal transplantation. My hope is that a preventative treatment to prevent CEC loss could be deployed into poor communities to help to prevent corneal blindness and thus to eliminate a good proportion the current need for expensive and inaccessible surgeries.
The second project to receive seed funding from the Tej Kohli Cornea Program will focus on eliminating corneal pain. A treatment to eliminate corneal pain remains one of the unmet needs in Ophthalmology. The research project will use novel drugs released by contact lenses to treat ocular surface pain and overcome the need for opioids when treating severe eye pain. Currently there are no FDA-approved products that eliminate corneal pain, and as a result, patients are commonly prescribed oral opioids to treat post-operative corneal pain.
A platform technology based on contact lenses that provide slow release of compounds has already been developed; and specialized pro-resolving mediators(‘SPM’) have been shown to actively resolve inflammation in a variety of acute and chronic inflammatory diseases. However, the effect of SPMs on pain have yet to be tested on the cornea. Therefore, the goals of the research project are to perform vitro studies to identify an SPM to treat eye pain, and to then incorporate that SPM into drug-eluting contact lenses.
I have high hopes that both of these projects will use their seed funding to prove their viability, and that they will ultimately contribute to the elimination of needless corneal blindness in poor communities. It is only through major scientific innovations borne from this kind of innovative research that we can move toward a world where nobody is needlessly blind because of poverty. And as seed projects like these ‘prove their worth’, I am prepared to keep doubling down on their efforts with additional funding so we can eliminate corneal blindness by 2035.
For more information on Tej Kohli as a philanthropist visit tejkohliruit.com and to read more of his views go to his Medium.
To read about Tej Kohli as an investor visit Kohli Ventures.
Find out more about Tej Kohli: Tej Kohli the technologist investing in human triumph, Tej Kohli the philanthropist trying to cure the developing world of cataracts and Tej Kohli the London tycoon with a generous streak.
| Follow: Twitter | Instagram | LinkedIn | Facebook | YouTube |



Comments ()